May 2020--As COVID-19 cases continue to be reported across the country and around the globe, many dental team members are asking, “Is it safe to see patients?”
“Yes, I think it’s safe to see patients today, provided we have the proper PPE and that we don’t rush back to practice,” said Linda Harvey, RDH, MS. Linda is a licensed Healthcare Risk Manager, author, and well-known regulatory compliance expert with 30 years of experience in providing quality assurance / patient safety perspectives for dental healthcare professionals and state licensing boards.
“We’re all eager to get back to taking care of our patients and being with our team members. We just have to take it slow and steady, take the time to prepare to have the office ready, and make sure everyone knows what is going to happen.”
Linda Harvey talked to Patient Prism CEO Amol Nirgudkar about the steps that dental practices should take.
You can also click here to download a guide that you can print and share with your team.
Dental Practices Changes to Increase Patient Safety
In the video, she outlines several steps that can be implemented to reduce the risk of infection, including:
- Pre-screening phone calls to confirm the patients’ health
- Teledentistry consultations to gain advance knowledge of the patients’ concerns and reduce the amount of time in the office
- Asking all team members and patients to wear face coverings
- Limiting who can accompany the patient into the practice
- Asking patients to remain in their cars until they can be seen
- Explaining physical distancing measures that have been implemented
- Removing beverage stations, magazines, and other community property from the waiting room
- Adding hand sanitizer stations in patient-facing areas
- Temperature checks for both team members and patients
- Enhanced Personal Protective Equipment (PPE) for team members
- Creating a list of answers for safety-related questions that patients may have
Linda Harvey stresses the need to document the protocols and processes you have in place, and assign people to be held accountable. For example, who will be in charge of conducting temperature checks and entering the results into patient files? Who will be responsible for disinfecting the common areas every half-hour?
PPE for Dental Practices During COVID-19
Both OSHA and the CDC recommend dentists and clinical team members wear N95 masks while performing dental services. The ADA released a chart showing the different levels of masks, the level of protection each provides, and each one’s limitations. Click here to view.
The dentist and team members should have an honest conversation about the Personal Protection Equipment (PPE) they’ll be using during this time. This will be different for everyone. The front desk team may not be used to wearing masks and gloves. The clinical team may not be used to wearing the level of PPE your team decides to implement, including form-fitted N95 or KN95 masks, face shields, scrub caps, isolation gowns, and shoe coverings.
It will physically take longer to change in-between patients and to clean the rooms, so practices may want to update their scheduling protocols. Many dental practices are extending hours and opening on weekends in order to allow for physical distancing and to accommodate their patients who may not be able to take time off from work or who cannot find childcare during the normal workday.
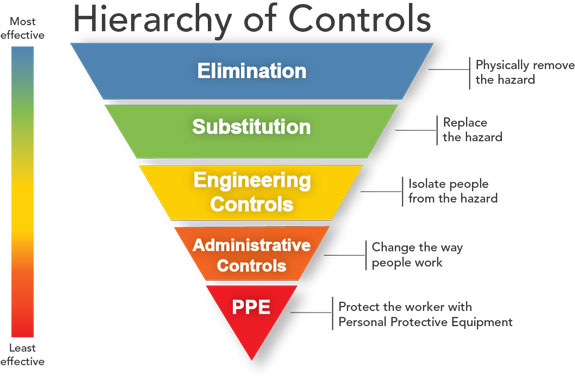
Hierarchy of Controls for Reducing Infection Risk
PPE is just the beginning, said Linda Harvey. She shares the CDC Hierarchy of Controls chart which shows the additional steps dentists and team members should take to reduce the risk of COVID-19 and other infections.
“PPE is really the lowest level of protection because of all the aerosols and transmissions,” said Harvey. “Then we move up that hierarchy to work practices and engineering controls. That where doctors need to decide if they need extra oral suction devices, a more sophisticated high vacuum system, aerosol-control purification systems and HEPA filters, et cetera.”
Communicating with Patients
It’s more important than ever to be clearly communicating with your patients, both on the phone before their visit and once they arrive.
An email announcing your safety protocols, pre-screening phone calls, and a door sign letting them know the protocol for entering your practice are just a few ways dental practices can be informing their patients of the changes they’ll see.
Social media videos and safety-focused messaging on your website and in your advertising are other ways you can let people know it’s safe to come to your practice.
Create a list of all the questions you think your patients might have and write out the answers so everyone in your practice uses the same phrasing to address concerns.
“Sometimes we can become defensive when patients ask about our sterilization processes,” said Harvey. “Now we have to be able to answer those questions confidently. If you don’t know the answer, simply say, ‘That’s a good question, Mrs. Jones. Let me get the answer for you.’ We need to be providing compassionate customer service now more than ever.”
Additional Resources
ADA: Return to Work Interim Guidance Toolkit and ADA.org/virus
CDC: Interim Infection Prevention and Control Guidance for Dental Settings During the COVID-19 Response
OSHA: Dentistry Workers and Employers COVID-19 Control and Prevention
For more interviews with experts, training resources, and guides, visit Academy.PatientPrism.com.
Subscribe to our blog for the latest updates
By submitting this form you will be receiving our latest updates on post. We're committed to your privacy. Patient Prism uses the information you provide to us to contact you about our relevant content, products, and services. You may unsubscribe from these communications at any time.
- Recent
- Popular











